My friend and colleague, Dr. Lani Simpson - Author: Dr. Lani's No Nonsense Bone Health Guide, is my guest blogger this month.
Fractures: Is Anyone Listening?
There are many types of fractures; a stress fracture is one of them. A stress fracture can be a normal response to repeated stress upon normal bone. A good example of this is a stress fracture that occurs when an athlete who is preparing seven days a week for a triathlon or a backpacker carrying a very heavy backpack and walking for miles. These stress fractures are most commonly seen in the bones of the feet and ankles. However, stress fractures can occur almost anywhere in the body and they can be normal or abnormal, which can indicate underlying bone pathology.
There are two types of stress fractures
- Fatigue fracture, which results from abnormal stresses on normal bone.
- Insufficiency fracture, which results from normal stresses on abnormal bone.
Other terms for insufficiency fracture can include low force or non-traumatic fracture or fragility fracture. Reports from radiologists tend to use insufficiency fracture.
INSUFFICIENCY FRACTURES
Insufficiency fractures (IFs) can occur with many bone diseases and conditions that weaken bone tissue. There is growing evidence that IFs are linked to long-term use of the most popular osteoporosis medications.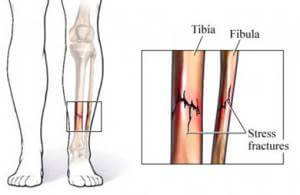
The focus of this article is insufficiency fractures that can occur following long-term use of the most commonly prescribed osteoporosis medications, Bisphosphonates (BP). This drug category includes: Fosamax (Alendronate), Actonel (Residronate), Boniva (Ibandronate), Reclast (Zoledronic acid) and many others. Another drug, Prolia (Denosumab) can also result in these fractures if used for an extended period of time.
Drugs to treat osteoporosis are classified as anti-resorptive (suppress bone breakdown) or anabolic (bone building). Currently there is only one FDA-approved medication in the category of anabolic and that is Forteo. All the rest are anti-resorptive and suppress bone break down. Most people treated for osteoporosis are taking a BP. Prolia is another anti-resorptive that can result in poor bone quality over time.
An insufficiency fracture indicates that a bone or bones are excessively weak. This could be caused from breast cancer or prostate cancer that has metastasized to bone or severe osteoporosis, or some other form of pathology that has weakened bone tissue.
Before we go on, it is important to understand how our bones stay healthy throughout our lifetime. This amazing process is called bone remodeling. The following explanation is from my book: Dr. Lani’s No-nonsense Bone Health Guide.
“Like a never-ending New Year’s celebration, your bones undergo a process of throwing out the old and welcoming the new right below the surface of your skin and muscles. This process—called “bone remodeling”—is a continuous cycle that recurs throughout your lifetime. It is designed to keep your skeletal structure healthy and supple by getting rid of old bone and laying down new bone. As we age, the remodeling becomes less effective, so that by the time we are in our eighties and nineties our bone is more brittle. It is possible, however, to slow down this particular aging process by eating healthy food and exercising.
Bone remodeling primarily depends on the work of two types of bone cells: osteoclasts and osteoblasts. The job of osteoclasts is to remove old bone (through a process called resorption), and the job of osteoblasts is to lay down new bone”
Here is a simple way to remember which type of bone cell does what:
- OsteoClasts—Chew up
- OsteoBlasts—Build up
How do Bisphosphonates and Prolia act on Bone?
They suppress osteoclasts. So, if the medication is taken for a long period of time, I think even a non-scientist would guess that one could end up with a bunch of old, broken down bone. Remember, osteoclasts remove old, damaged bone.
Studies have shown that long-term use (over five years) can result is osteonecrosis of the jaw (areas of bone death) and Atypical Femur (thigh bone) Fractures (AFF) of the strongest bone in the body. Because both of these conditions are rare, doctors began to notice an uptick in both conditions in people who had used Fosamax for an extended period of time. However, we are told that the percentage of these conditions is small. I do not feel that it is as small as we are led to believe. In fact, I recently did a webinar with Jennifer Schneider, MD who herself experienced a complete fracture of her femur following shifting her weight from one leg to the other. Since that time she’s made it her life’s mission to educate the public about this devastating side effect of long-term use of BPs, and she has presented to the FDA twice regarding Atypical Femur Fractures.
This type of fracture, where the femur breaks non-traumatically is an insufficiency fracture. Dr. Schneider also has a group of 200 people who have experienced such fractures and have managed to find her. So, I wonder, when a patient presents with one of these types of fractures, how often are they really being reported. Because someone with osteoporosis could sustain such a fracture, it may simply be attributed to osteoporosis. However, this should not happen in people who were perfectly normal prior to the use the Fosamax with no previous non-traumatic fractures and who are otherwise healthy. The reason I’m singling out Fosamax is because that was the first BP that came on the market and it was used the longest, so the side effects showed up with Fosamax early on. However, all BPs and Prolia essentially act the same way, suppressing osteoclasts. Dr. Schneider conducted a retrospective study on her group (Just over 100 people at the time) who sustained non-traumatic atypical femur fractures. In this group 35% went on to have a second AFF of the OTHER femur. She also found that many in her group also sustained metatarsal (long foot bone) fractures. I also found several case studies pointing to the metatarsal insufficiency fractures as a concern for long-term use of BPs.
Warnings about Bisphosphonates and Prolia
The makers of both drugs warn of Atypical Femur Fracture, which is an insufficiency fracture and osteonecrosis of the jaw. However, nowhere could I find the term insufficiency fracture mentioned on their label or on the company website. I was able to find it on the FDA site along with plenty of case studies pointing to other areas of the body where bones simply failed “for no reason”.
Now, I am hoping to bring much more awareness to insufficiency fractures. For example, I have interviewed one patient and analyzed her history of multiple insufficiency fractures in her pelvis and sacrum. She started on Fosamax as a prevention for osteoporosis, meaning that she did not even have osteoporosis when she began taking it. What’s more, she never sustained a fracture in her life and was a very healthy active person. Then she had her, “three months from hell” as she puts it. The pain she felt in her pelvis, she said, was beyond the pain of giving childbirth. For a number of reasons, she was not diagnosed as having fractures for over a month. The way that she learned that she had sustained multiple pelvic and sacral fractures was when her doctor’s office assistant called to tell her the bad news.
When somebody sustains an insufficiency fracture (low-trauma or NO trauma)
it should be considered serious and could be an emergency.
Insufficiency fractures can occur in any bone of the body with just the body weight itself being enough to result in such fractures. The pelvis, sacrum and spine are common areas for insufficiency fractures. These fractures may not show up on x-rays, but an MRI or CT scan of the area in question can diagnose these painful fractures.
It is important to note that some doctors are somewhat aware of the bisphosphonates resulting in such fractures. In order to help their patients avoid one of these fractures they are switching patients to a different bisphosphonate or to Prolia, which is not really a switch at all, and in fact, is contraindicated. As mentioned earlier, bisphosphonates slow down bone loss by inhibiting the action of osteoclasts from removing old damaged bone. Prolia has a different path to slow down bone loss, but essentially it does the same thing, it suppresses osteoclasts.
THE PROBLEM REGARDING THE DIAGNOSIS AND PROPER REACTION TO INSUFFICIENCY FRACTURES (IFs):
Many doctors do not fully understand what exactly an insufficiency fracture is or that prolonged use of these medications is associated with insufficiency fractures. If they do not understand their significance, they are not being reported. Some time ago, I was working as a densitometrist for an osteoporosis bone density testing center. In most centers, patients fill out a questionnaire and they are asked if they have “ever” had a fracture. In this center if they answer yes, the report defaulted to insufficiency fracture. In other words, that was automatically inserted into the report! Now imagine a doctor who does understand the meaning – they will prescribe a medication immediately – Egad! When I saw this I had them change the wording immediately on my reports and taught the tech how to ask the right questions to determine if the fracture was significant. This is important because it will up your fracture risk in the report. So, if someone broke a toe or a finger that does not count as an osteoporosis related fracture. If they fractured a bone slamming their bike into a tree – that also does not count. However, if they fractured their forearm with little or no trauma, that does count. Or, if they fractured a metatarsal with – no-trauma that could be an insufficiency fracture. Sometimes you and the doctor must dig deeper.
Actual wording on company websites
Warning Labels on Prolia and Fosamax Medication
PROLIA (Denosumab):
- Severe jaw bone problems
- Unusual thigh bone fractures
Fosamax (Alendronate)
- Osteonecrosis of the Jaw has been reported
- Atypical Femur Fractures have been reported
Warning labels for Prolia and Fosamax as well as all BPs include osteonecrosis of the jaw and atypical femur fractures as possible unwanted side effects. NOWHERE is the term insufficiency fracture mentioned. Let’s think about this for a moment. A patient gets a bone density scan ordered by a general practitioner who continues to prescribe it for the next 5 years. All of the sudden the patient feels horrible pain in their sacrum. Some months later an MRI is ordered and the fracture is identified. How many doctors or radiologists do you think would connect the dots?
Dr. Lani's Website: https://www.lanisimpson.com
My question for you.
When it comes to choosing the right foods to optimize your bone health, what is the single biggest challenge, frustration or problem you’ve been struggling with?
Please let me know so I can write content that meets your needs.
Plus I have wonderful alkaline salad dressing waiting for you on the other side to thank you for your time 🙂.
Click here to share your challenges ----> HERE
References
Atypical Fractures of the Femoral Diaphysis in Postmenopausal Women Taking Alendronate N Engl J Med 2008; 358:1304-1306 March 20, 2008 Brett A. Lenart, B.S. Dean G. Lorich, M.D. Joseph M. Lane, M.D. Weill Cornell Medical College, New York, NY 10021 https://www.nejm.org/doi/full/10.1056/NEJMc0707493
Osteoporos Int. 2015 Nov 10.
Bilateral distal fibula fractures in a woman on long-term bisphosphonate therapy.
“Atypical femur fractures: 81 individual case histories.” by Jennifer P. Schneider, William B. Hinshaw, Christina Su, and Phyllis Solow, 2012. Journal of Clinical Endocrinology and Metabolism, 97:4324-4328.
Murray JC1, Audet MC2,3, Bédard M1, Michou L4,5,6. https://www.ncbi.nlm.nih.gov/pubmed/26556740
“Bisphosphonates and low-impact femoral fractures: Current evidence on alendronate-fracture risk.” Jennifer P. Schneider Geriatrics 64:18-23. 2009.
Journal of Bone and Mineral Metabolism
September 2007, Volume 25, Issue 5, pp 333-336
Pelvic insufficiency fracture associated with severe suppression of bone turnover by alendronate therapy
https://link.springer.com/article/10.1007/s00774-007-0771-y
Kaplan P. Musculoskeletal MRI. W B Saunders Co. (2001) ISBN:0721690270.
Burnet S, Mahadevan G, Lee A et-al. Sacral insufficiency fracture–a case of post-coital back pain. Rheumatology (Oxford). 2001;40 (9): 1065-6. doi:10.1093/rheumatology/40.9.1065 – Pubmed citation
Chen C, Chandnani V, Kang HS et-al. Insufficiency fracture of the sternum caused by osteopenia: plain film findings in seven patients. AJR Am J Roentgenol. 1990;154 (5): 1025-7. AJR Am J Roentgenol (abstract) – Pubmed citation
Burgener FA, Kormano M, Pudas T. Bone and Joint Disorders. Thieme Medical Pub. (2005) ISBN:1588904458.
Porrino JA, Kohl CA, Taljanovic M et-al. Diagnosis of proximal femoral insufficiency fractures in patients receiving bisphosphonate therapy. AJR Am J Roentgenol. 2010;194 (4): 1061-4. doi:10.2214/AJR.09.3383
Burgener FA, Kormano M, Pudas T. Bone and Joint Disorders. Thieme. (2006) ISBN:1588904458.
Greaney RB, Gerber FH, Laughlin RL et-al. Distribution and natural history of stress fractures in U.S. Marine recruits. Radiology. 1983;146 (2): 339-46. Radiology (abstract) – Pubmed citation
Let Me Support Your Bones
Get Customized In-Depth Private Session
Book a Private Coaching with Irma Now
Join Our Amazing Bone Tribe Community
Get the support & information you need to live fearlessly with your bones diagnosis
From my bones to yours,
Irma Jennings, INHC
Your Holistic Bone Coach
[email protected]